Gestational surrogacy is not a single medical event but a carefully sequenced clinical pathway integrating reproductive endocrinology, embryology, obstetrics, and preventive maternal–fetal medicine. Each phase is designed to control variables, optimize implantation potential, reduce maternal risk, and support fetal development within a highly monitored environment. Understanding this structure transforms the process into a scientifically managed and medically predictable journey.

Pre-Cycle Medical Qualification: Risk Assessment and Reproductive Readiness
Before medications begin, the surrogate undergoes a comprehensive evaluation functioning as a predictive model for pregnancy safety and success. This is a clinical risk-stratification process rather than a simple checklist.
Core components include:
- Detailed obstetric history with outcome analysis
- Review of prior delivery methods and uterine recovery
- Endocrine and metabolic screening
- Infectious disease panel per FDA reproductive tissue guidelines
- Uterine cavity assessment via saline sonogram or hysteroscopy
- Ovarian suppression response testing when indicated
The objective is to confirm demonstrated reproductive capacity, identify implantation risks, and establish a baseline for individualized medication protocols.
Endometrial Preparation and Cycle Control
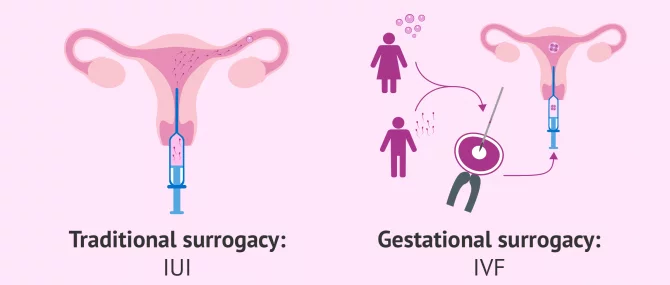
Gestational surrogacy requires precise hormonal orchestration. Natural ovulation is often suppressed so the uterine environment can be fully controlled and synchronized with embryo development.
- Estrogen administration to promote endometrial proliferation
- Serial ultrasound measurement of endometrial thickness and pattern
- Serum estradiol monitoring for adequate absorption
- Timed progesterone initiation to define the implantation window
This controlled simulation of the luteal phase replicates optimal physiologic conditions and is a key determinant of implantation success.
Embryo Transfer: Precision Without Invasiveness
Embryo transfer is a high-precision procedure performed under ultrasound guidance. A catheter is gently advanced through the cervix, and the embryo is placed at a measured position within the uterine cavity.
- Atraumatic technique to prevent uterine contractions
- Controlled catheter placement depth
- Minimal uterine manipulation
- Optimized embryo–endometrium synchrony
Implantation depends on the interaction between endometrial receptivity, embryonic competence, and progesterone exposure duration.
Luteal Phase Support and Implantation Physiology
After transfer, pregnancy relies on exogenous hormonal support until placental autonomy develops.
- Continued progesterone supplementation
- Estrogen support when indicated
- Activity guidance per clinic protocol
Rising beta-hCG levels indicate trophoblastic activity and allow early identification of implantation success or failure.
Early Gestational Surveillance

The fertility clinic maintains supervision through early first trimester monitoring:
- Serial quantitative beta-hCG testing
- Ultrasound confirmation of intrauterine gestation
- Crown–rump length measurement for dating
- Fetal cardiac activity detection
This phase confirms viability, excludes ectopic pregnancy, and determines safe transition timing to obstetric care.
Transition to Obstetric Management
After release from the fertility clinic (typically 8–10 weeks), care transitions to an obstetrician or maternal–fetal medicine specialist.
- Trimester-based prenatal surveillance
- Fetal anatomic evaluation
- Gestational diabetes screening
- Hypertensive disorder monitoring
- Cervical length assessment when risk factors exist
Surrogate pregnancies often include enhanced coordination between medical teams and intended parents, as well as structured documentation for legal planning.
Evidence-Based Technologies Improving Outcomes
- Preimplantation genetic testing (PGT) to reduce aneuploid implantation
- Frozen embryo transfer cycles for optimized endometrial preparation
- Endometrial receptivity analysis for personalized progesterone timing
- Elective single embryo transfer to reduce multiple gestation risk
These technologies move gestational surrogacy from probability-based treatment toward data-driven reproductive medicine.
Labor, Delivery, and Postpartum Coordination
Delivery is both a medical and logistical event. Planning includes:
- Mode of delivery based on obstetric history
- Hospital coordination regarding legal parentage
- Neonatal care transfer procedures
- Structured postpartum recovery planning
Postpartum care evaluates uterine involution, hormonal stabilization, surgical recovery when applicable, and lactation management based on prior agreements.
Conclusion: Surrogacy as Coordinated Reproductive Medicine
Gestational surrogacy represents a highly coordinated model of reproductive medicine. Through structured screening, hormonal control, continuous monitoring, and evidence-based technology, the process maximizes safety and predictability for both surrogate and intended parents. When managed within a professional medical framework, surrogacy becomes not an uncertain event, but a carefully guided clinical pathway.
